This article is dedicated to Hildegard E. Peplau and her life so that we may come to fully appreciate the impact that she had on our nursing profession. She provided an education that encourages interactions with our patients to our fullest potential. She is the reason why we as nurses can assess patients with questions and be the answer to the questions that patients have. Before her, patients weren’t people nurses interacted with. So this is the life and story of Hildegard E. Peplau, the woman who advocated for patient interaction and made patient-nurse interactions a core nursing principle.
Hidegard E. Peplau (September 1, 1909 – March 17, 1999), was an American nurse and revolutionized the academic paradigm of nursing theory by introducing patient-nurse relations to the nursing process. She considered patient interactions to be fundamental to the nursing process and this article focuses on her life and explains her theory about nurse-client interactions and why her theory matters today.
Hildegard Peplau Biography
Early Life
Hildegard was born September 1, 1909, in Reading, Pennsylvania as the second child of six children to German immigrant parents. Gustav was her illiterate yet hard-working father and Otyllie was her mother who was harsh and held high standards. Hilda was described as determined and observant  as a child. She was visionary and although higher education was not a topic of discussion at home, she sought to have a career and become beyond what was normally expected of a traditional woman. She decided a career in nursing because nursing was one of the few careers attainable by women at the time and also she saw how much death and illness impacted people during the flu epidemic of 1918, where she even saw people jump out of windows from delirium.
as a child. She was visionary and although higher education was not a topic of discussion at home, she sought to have a career and become beyond what was normally expected of a traditional woman. She decided a career in nursing because nursing was one of the few careers attainable by women at the time and also she saw how much death and illness impacted people during the flu epidemic of 1918, where she even saw people jump out of windows from delirium.
But in the early 1900s, nursing schools were missing a few ethical principles, where there was no autonomy because hospitals completely controlled nursing schools, and nurses were trained with injustice as nursing students were discouraged from a formal education such as learning from books. Women in nursing were treated with injustice as they were exploited and used as dispensable labor in both school and work settings.
Career
In 1931, Peplau graduated from the Pottstown Hospital School of Nursing and started her nursing career as a staff nurse in Pennsylvania and New York City.
As she worked at New York University’s summer camp, she got recommended to work at Bennington College in Vermont and accepted the offer. Working at Bennington was a pivotal point in Peplau’s life because that is where she transitioned into the field of interpersonal psychology, where she not only got a bachelor’s degree in interpersonal psychology but where she also studied under known experts such as Eric Fromm, Frieda Fromm-Reichman, and was exposed to Sullivan, whose work became her lifelong and signature pursuit of interpersonal psychology in the nursing field.
After graduating with a bachelor’s degree in psychology, Peplau served in the Army Nurse Corps from 1943 to 1945 and she was  stationed in England, by the American School of Military Psychiatry. This was another pivotal point in her life because this was where she was introduced to the influential men of British and American psychiatry who she would collaborate with after the war to reform the United State’s mental health system, through the National Mental Health Act of 1946. Serving in the Army Nurse Corps became her leverage in influencing mental health reform that brought more humane treatments for the mentally ill in the United States.
stationed in England, by the American School of Military Psychiatry. This was another pivotal point in her life because this was where she was introduced to the influential men of British and American psychiatry who she would collaborate with after the war to reform the United State’s mental health system, through the National Mental Health Act of 1946. Serving in the Army Nurse Corps became her leverage in influencing mental health reform that brought more humane treatments for the mentally ill in the United States.
Peplau became certified in psychoanalysis by the William Alanson White Institute of New York City and got her master’s and Ph.D. from Teachers College, Columbia University. Early 1950’s, Dr. Peplau taught her first classes for graduate psychiatric nursing students at Columbia University. And from 1954 to 1974, Dr. Peplau served as faculty of the College of Nursing at Rutgers University, where she developed her own graduate-level clinical program in psychiatric nursing.
Dr. Peplau advocated for patient interactive interventions through her writing, speeches, presentations, and clinical workshops. Throughout the 1950s and 1960s, Dr. Peplau conducted seminars in hospitals and introduced interpersonal relation concepts to help nurses better identify patient needs and deliver solutions with relevant and effective manners. She revealed how these concepts prepare nurses to improve client-nurse relations to better assess and meet client needs throughout different settings, such as group, family, or individual therapies.
In her later years, Peplau was a consultant to the World Health Organization, flew throughout Latin America, Belgium, Africa, and the United States as a guest professor for universities and she advocated for the development of nursing practice through research. She had also served as an advisor to the U.S Surgeon General, the U.S Air Force, and the National Institute of Mental Health. She was involved in various policy-making groups and served as president of the American Nursing Association from 1970-1972 and as vice president from 1972-1974. After she retired from Rutgers University, she lived in Belgium from 1975-1976 as a visiting professor to help create the first graduate nursing program in Europe for the University of Leuven.
Death
Peplau passed away peacefully at her home in Sherman Oaks, California in 1999. She had one daughter named Anne Peplau, who she birthed after being involved in an extramarital affair in 1944, and Peplau spoke highly of Anne’s father before her death. Anne Peplau was born in 1945, was raised by a single mother, and grew up to be a psychology professor at UCLA where she strongly advocated for scientific research and was also influential in the scientific literature.
Hildegard Peplau’s Interpersonal Relations Theory
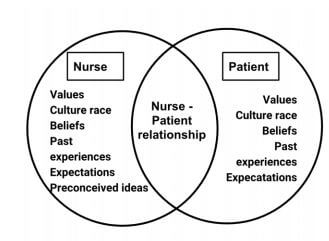
Dr. Peplau introduced her interpersonal relationship theory in her book Interpersonal Relations that she published in 1952 where she emphasized patient-nurse interactions and believed that shared experiences with patients were foundational to nursing practice. Her theory recognized a give-and-take nurse-client relationship that many thought to be revolutionary. She shifted the nursing paradigm about treating patients with an emphasis on establishing a nurse-client relationship, instead of passively delivering treatment and following doctor’s orders.
Dr. Peplau conceptualized patient-nurse interactions and believed that any nurse can create a shared experience with a client by observing and describing a client’s need, formulating, interpreting, and validating a solution to implement and meet the client’s need. This revolutionary process empowers the client to be a part of the solution, not only producing more direct and accurate solutions but also develops personal growth for both client and nurse. This process produces personal growth that shapes the role of the nurse defined in Peplau’s model and produces interactive phases between client and nurse identified as Peplau’s Developmental Stages that can be recognized in today’s nursing process.
Peplau’s Six Nursing Roles Model
Peplau studied client relations and identified roles that occupy relations that are still evident in today’s nursing process. Peplau created a model of six types of roles that describes the different types of interpersonal roles that exist in nursing care.
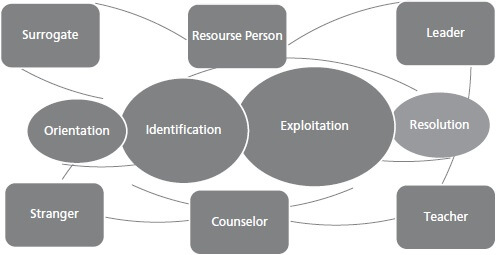
The goal of the model is to identify the roles established within nurse-client interactions to guide nurses to establish a role that is most appropriate for providing a need. Nurses can leverage this model to create a role that better suits delivering a solution.
The Stranger role has the lowest degree of intractability compared to the other roles. The client and nurse communicate through respect and courtesy for one another. The client is independent of the nurse’s care and both client and nurse should respect that independence. With this role, an atmosphere of mutual trust and respect is crucial. This role can be seen in nursing today within nurse-client interactions during a screening process. The client and nurse interact as this role when the nurse takes patient vital signs. While taking vitals, the nurse may occupy the stranger role where there is little to no interactions besides having a respectful environment.
The Resource role is where the client asks questions and the nurse is responsible for delivering information. The nurse is expected to be straightforward, providing constructive answers. There is an exchange of questions and answers between the client and nurse and the nurse is expected to be the source of solutions. The resource role is seen often in businesses, where customers need answers for a product and are dependent on the service to provide the most relevant answers. A nurse may fulfill a resource role when delivering information to a patient before discharge.
The Teaching role is established when the nurse is able to change the client’s behavior through suggestions or instructions. The client trusts that the nurse has in consideration the best interest of the client. As rapport is required for this role, the nurse should be responsible for providing accurate and relevant instructions. This role is often seen in sports training, where the trainer leads the client into a routine. In today’s nursing, when nurses are in a position of teaching, they should recognize that rapport is important and that this role is focused on producing results with directions or instructions.
The Leadership role involves the nurse empowering the client to make his or her own decisions. The nurse should have the best interest of the client while enabling the client to make decisions. Nurses in this role should be engaging because client empowerment requires active participation. In today’s nursing care, nurse practitioners occupy this role as clients are empowered to decide which provider they want to select.
The Surrogate role develops as the client projects emotions of past feelings for his or her mother towards the nurse because the client is dependent on the care of the nurse. In this case, the nurse takes up a motherly role and the client should be reminded that this relationship is temporary and not like the one with his or her mother to avoid disappointment. There should be a clarification on which activities require the patient’s independence, interdependence, or dependence on the nurse. In intensive care units or nursing homes, patients may become dependent on nursing care where a nurse becomes a surrogate role.
The Counseling role is interactive, empathic, and is the emphasis of nursing. The client and nurse interact with empathy, such as how friends or family members interact. This role should be seen in the majority of today’s nurse-client interactions as the nursing process should progress with the nurse treating patients as they would a friend or a family member. This role should progress into memorable and integrative experiences.
All six roles can be seen throughout today’s nursing process and can be leveraged to appropriately and accurately deliver solutions. As a nurse, you can apply for these roles as functions that you can apply to replay to the patient with a solution. Respect, information, instructions, role clarity, empowerment, and empathy are the six responses a nurse can use when delivering a need to promote personal growth and to improve patient-nurse experiences.
Development of interpersonal Nurse –Client relationship
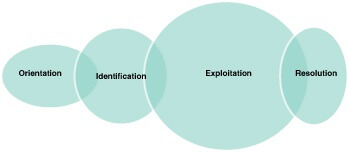
The orientation phase is the initial phase of Paplau’s interpersonal phases. This phase is crucial because this is when the nurse initiates the nurse-client relationship. The nurse should introduce him or herself to the client to explain what he or she is there to do. This is when the nurse sets boundaries and first impressions. The patient should understand that the nurse is there to help the client, be patient-centered, and develop a professional relationship rather than a social one. This phase must have the patient feel genuinely cared for to establish a nurse-client relationship.
The identification phase is when the nurse identifies the problems that are associated with the patient. This is when the nurse asks questions regarding the patient’s situation and goals to assess the patient’s needs and develop a nursing care plan. The client should begin to trust the nurse and have a sense of safety.
The exploitation and working phase is when the client and nurse work to restore the client to the client’s full potential. In this phase, the client should fully trust the nurse and fully utilize the nurse as a resource. The client approaching the nurse as a resource is a sign that the client has advanced to the working phase. The client and the nurse proceed to accomplish time-specific discharge and termination goals.
The resolution or termination phase occurs when the patient is discharged, restored to self-reliant condition, or when treatment goals have been met. The client-nurse relationship terminates after a short or long-term relationship, and the relationship is summarized without complexities. This final step is when the nursing process is terminated and evaluated.
There are limitations to Peplau’s theory of relations for a couple of reasons. Peplau’s theory of interpersonal relations does not apply to all patients. Her theory cannot be applied to unconscious patients and patients who do not believe they have a need that can be resolved. Also, this theory lacks considering social services as a nursing intervention and does not emphasize health promotion and maintenance as an intervention.
These phases of client-nurse interpersonal relations were revolutionary and are still applied today in nursing. Today’s nursing process is heavily influenced by Peplau’s theory and these phases and roles are still observable today in modern nursing practices. Peplau’s integration of nursing and psychology has created a foundational principle of modern-day nursing.
Peplau believed that the nursing process should involve two or more people working together for a common goal to understand and identify difficulties through interpersonal interactions to result in therapeutic effects. Peplau believed nursing care should be a healing process, where both nurses and patients are involved to work for a common goal where they can both mature. Peplau created a nursing theory that involved patient interactions in a nursing process in hopes that both nurse and patient work together to discover healing through their relationship.
Peplau is recognized as the nurse of the century for her advocacy for patient-nurse interactions to develop into therapeutic solutions. Her life journey advocated the improvement of nursing care and nursing theory has progressed from her contribution. Future nurses can learn from Peplau’s theory and assist patients with the role most suited to provide the patient with the best response possible.