A virus with no definite source. A newly identified disease. An illness without a vaccine. A disease with no treatment. A disease that is contagious. Knowing that there’s no place and no one here on earth could be possibly exempted from the outbreak of coronavirus – the outbreak scares the world.
Scares spread rapidly all throughout the world affecting particularly Saudi Arabia, where the outbreak started. Recently, it was reported that four doctors from the main hospital in the western city of Saudi Arabia have resigned after they refused to treat patients with MERS-CoV due to the fear of infection and some facilities have been temporarily shut down last month after numerous health staffs got infected with the virus (Times of Oman 2014).
How scary is the MERS-CoV? Up to date, MERS disease mortality surged to 40% since its outbreak in 2012 and is considered deadlier but less transmissible compare to SARS or Severe Acute Respiratory Syndrome (Times of Oman 2014).
May 9, 2014 – Public Health of Ontario reported that there are seventeen (17) countries, which are affected with the illness caused by MERS-CoV such as Egypt, France, Germany, Greece, Italy, Jordan, Kuwait, Malaysia, Oman, Philippines, Qatar, Saudi Arabia, Tunisia, United Arab Emirates, United Kingdom, United States of America and Yemen (Public Health Ontario 2014). A week after, Lebanon and the Netherlands were included in the list (WHO 2014a).
As of May 15, 2014 – there are 572 laboratory-confirmed cases of MERS-CoV infection with 173 mortality rates around the globe have been officially reported to World Health Organization; 18 new cases globally were added from the previous updates; and 58 laboratory-confirmed cases that are reported came from Saudi Arabia between May 5-9, 20014 (WHO 2014a).
The MERS-CoV
The Centers for Disease Control and Prevention defined MERS-CoV or the Middle East Respiratory Syndrome CoronaVirus as a form of viral infection affecting the respiratory system (CDC 2014a). CDC reported that the novel coronavirus found in SARS is different from the coronavirus of MERS as both having different types of coronavirus strains (CDC 2014a). Moreover, MERS is characterized as SARS-like virus because both strains of coronavirus are found in bats and both syndromes shared the same symptoms such as flu like symptoms, which are severe and acute during onset (CDC 2014a; WHO 2014b).
People who are affected by the virus usually present with fever, chills, cough and shortness of breath, and/or difficulty of breathing (dyspnea) (WHO 2014a). The illness becomes fatal due to severe acute respiratory infection and is associated with renal failure (Public Health Ontario 2014).
Statistics revealed how contagious and deadly the coronavirus is. World Health Organization (WHO 2014b) reported that 1/3 of the people that were infected with MERS have died with fatal cases of severe respiratory symptoms involving the elderly and patients with previous serious medical problems.
Mode of Transmission and Illness Occurrence
Because of the small number of cases identified for each particular places, there is very limited information on transmission, epidemic issues, severity and clinical impact creating small patches to fill a big hole in the puzzle that creates craze and scare over MERS-CoV. Still, the mode of transmission is unknown (CDC 2014a; WHO 2014b; Public Health Ontario 2014).
Coronavirus is transmitted through close contact with infected persons (WHO 2014b). Though there is no available study yet to prove the transmission from infected animals, laboratory findings on animals such as bats and animals having the coronavirus strains (CDC 2014a; WHO 2014b), is enough reason for us to take extra precautionary measures in handling or contact to such animals.
Human to human transmission may be limited because of insufficient reported cases of family clusters infections and small incidence of household transmission which only occur in the United Kingdom, the Kingdom of Saudi Arabia, Tunisia, and Italy (Public Health Ontario 2014).
Reported cases of nosocomial infections occurred in France, United Arab Emirates, and Saudi Arabia; however, the nosocomial cases in France were linked to exposure to the countries of the Arabian Peninsula (Public Health Ontario 2014).
WHO reported that 75% of persons infected with coronavirus are secondary cases, implying that they have acquired the disease from other infected persons; and the majority of these cases are health care workers who acquired the disease from nosocomial infections (WHO 2014b).
Analyzing the geographical and economic state, Middle East, America and Europe are the greatest importers of health workers around the globe. While Asian countries like the Philippines and Malaysia are exporters of overseas workers. Migration and tourism can be the possible reasons for the spread of infections. Outbreaks are considered as nosocomial infections and exported cases through tourists, travelers, overseas workers, and pilgrims who might acquire the infection from environmental sources, infected animals, and persons (WHO 2014b).
However, WHO (2014b) reported that the occurrence of outbreaks follows a seasonal pattern with increasing incidence from March to April onwards in Saudi Arabia and UAE. Moreover, the largest outbreaks happened in 2013, which occurred from April to May in eastern Saudi Arabia (CDC 2014b). Exported cases from 2012-2014 reported that they have traveled to Saudi Arabia, Qatar and UAE (CDC 2014a; WHO 2014b). Minor and single cases appeared only throughout the year but outbreaks and epidemics fall during the month of April to May. On the contrary, in the study of Van Doremalen et al (2013) it was concluded that MERS-CoV was more stable at low temperature / low humidity environmental conditions and could still be recovered after 48 hours. This may suggest that transmission takes place in an indoor with a conducive environment viable for the coronavirus strains of MERS.
WHO advice
Based on the current situation and available information, WHO encourages all Member States to continue their surveillance for severe acute respiratory infections (SARI) and to carefully review any unusual patterns.
Infection prevention and control measures are critical to prevent the possible spread of MERS-CoV in health care facilities. Health-care facilities that provide for patients suspected or confirmed to be infected with MERS-CoV infection should take appropriate measures to decrease the risk of transmission of the virus from an infected patient to other patients, health-care workers and visitors. Health care workers should be educated, trained and refreshed with skills on infection prevention and control.
It is not always possible to identify patients with MERS-CoV early because some have mild or unusual symptoms. For this reason, it is important that health-care workers apply standard precautions consistently with all patients – regardless of their diagnosis – in all work practices all the time.
Droplet precautions should be added to the standard precautions when providing care to all patients with symptoms of acute respiratory infection. Contact precautions and eye protection should be added when caring for probable or confirmed cases of MERS-CoV infection. Airborne precautions should be applied when performing aerosol-generating procedures.
Patients should be managed as potentially infected when the clinical and epidemiological clues strongly suggest MERS-CoV, even if an initial test on a nasopharyngeal swab is negative. Repeat testing should be done when the initial testing is negative, preferably on specimens from the lower respiratory tract.
Health-care providers are advised to maintain vigilance. Recent travelers returning from the Middle East who develop SARI should be tested for MERS-CoV as advised in the current surveillance recommendations. All Member States are reminded to promptly assess and notify WHO of any new case of infection with MERS-CoV, along with information about potential exposures that may have resulted in infection and a description of the clinical course. The investigation into the source of exposure should promptly be initiated to identify the mode of exposure so that further transmission of the virus can be prevented.
People at high risk of severe disease due to MERS-CoV should avoid close contact with animals when visiting farms or barn areas where the virus is known to be potentially circulating. For the general public, when visiting a farm or a barn, general hygiene measures, such as regular hand washing before and after touching animals, avoiding contact with sick animals, and following food hygiene practices, should be adhered to.
WHO does not advise special screening at points of entry with regard to this event nor does it currently recommend the application of any travel or trade restrictions. – Source: World Health Organization, 15 May 2014. Available at: http://www.who.int/csr/don/2014_05_15_mers/en/
Treatment and Management
Up to date, there is no identified vaccine to prevent the illness and no specific treatments to cure MERS, medical care are usually palliative and supportive to help relieve the symptoms (CDC 2014a).
References
- Centers for Disease Control and Prevention (CDC). 2014a. Middle East Respiratory Syndrome (MERS). Available at: http://www.cdc.gov/coronavirus/mers/faq.html [Accessed: 03 May 2014].
- Centers for Disease Control and Prevention. 2014b. Press Release : CDC announces first case of Middle East Respiratory Syndrome Coronavirus infection (MERS) in the United States. Available at: http://www.cdc.gov/media/releases/2014/p0502-US-MERS.html [Accessed: 03 May 2014].
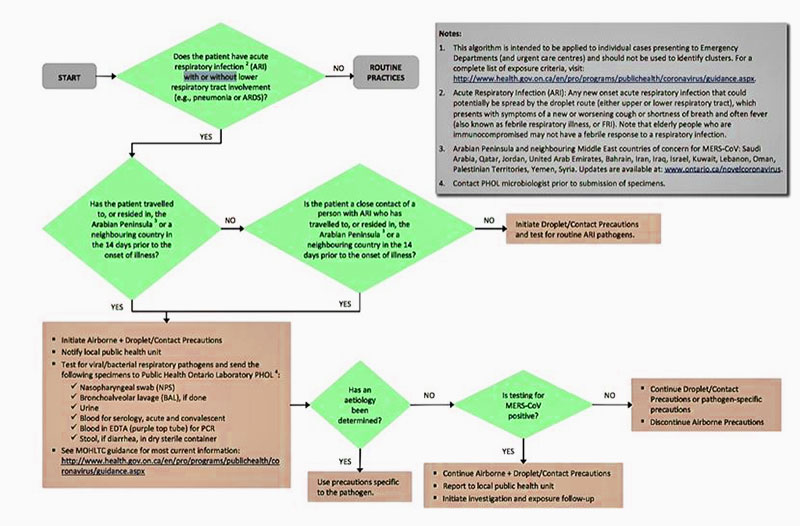
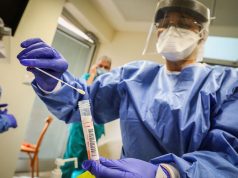
- Public Health Ontario. 2014. Tools for Preparedness: Triage, Screening and Patient Management for MERS-CoV Infections in Acute Care Settings, 3rd ed. Toronto, ON: Queen’s Printer for Ontario.
- Times of Oman. 2014. Saudi Hospital Head Sacked Over MERS Panic. Available at: http://www.timesofoman.com/News/33494/Article-Saudi-hospital-head-sacked-over-MERS-panic [Accessed: 08 May 2014].
- Van Doremalen, N., Bushmaker, T. and Munster, V.J. 2013. Stability of Middle East Respiratory Syndrome Coronavirus (MERS-CoV) Under Different Environmental Conditions. Eurosurveillance, 18(38)
- World Health Organization (WHO). 2014a. Global Alert and Response (GAR) : Middle East Respiratory Syndrome Coronavirus (MERS-CoV) Update. Available at: http://www.who.int/csr/don/2014_05_15_mers/en/ [Accessed: 16 May 2014].
- World Health Organization (WHO). 2014b. Global Alert and Response (GAR) : Coronavirus Infection. Available at: http://www.who.int/csr/disease/coronavirus_infections/MERS_CoV_RA_20140424.pdf?ua=1 [Accessed: 16 May 2014]