Chronic suppurative otitis media (CSOM) is caused by recurrent ear infections resulting in tympanic membrane perforation characterized by persistent foul-smelling otorrhea from the middle ear. Misconception on ear infection as related to poor hygiene and embarrassing foul-smelling ear discharges generates an erroneous notion of social stigma—which is one of the major causes of hearing loss in CSOM, since most of the cases are not reported and not diagnose earlier without immediate and appropriate treatment. Hearing loss is preventable if only immediate treatment is taken (Smeltzer & Bare, 2004; Acuin, 2004; Bonin et al., 2003).
In the report of Acuin (2004), prevalence surveys confirmed that the global burden of illness from CSOM affects 65–330 million individuals with draining ears, 60% of whom (39–200 million) suffer from significant hearing impairment. CSOM accounts for 28, 000 deaths and a disease burden of over 2 million DALYs. Over 90% of the burden is borne by countries in the South-east Asia and Western Pacific regions, Africa and several ethnic minorities in the Pacific rim. Mastoidectomy with or without tympanoplasty eradicates mastoid infection in about 80% of patients and may be combined with surgical drainage of otogenic abscesses. However, such treatment is costly and does not always lead to satisfactory hearing improvement, and is inaccessible in many developing countries.
Smeltzer & Bare (2004), defines chronic suppurative otitis media as the result of repeated episodes of acute otitis media causing irreversible tissue pathology and persistent perforation of the tympanic membrane. Chronic infections of the middle ear damage the tympanic membrane, destroy the ossicles, and involve the mastoid (Smeltzer & Bare, 2004, Acuin, 2004). CSOM may develop in elderly people who have had an asymptomatic or exacerbated chronic ear infection after URI or when water enters the middle ear during bathing or swimming. Chronic suppurative otitis media may be a complication of a retracted or perforated tympanic membrane. In elderly patients with otorrhea, squamous, and basal cell carcinomas should be considered (Acuin, 2004). Tympanic membrane perforation may be permanent, and the middle ear mucosa may become hypertrophic. In some patients, the inflamed, polypoid hypertrophic mucosa protrudes through the perforation into the external auditory canal as an aural polyp. A cholesteatoma may be present. Some cases are complicated by abscess formation or erosion into bone (Smeltzer & Bare, 2004).
Anatomy and Physiology of Sense of Hearing
The ear has external, middle and inner ear sections and provides the senses of hearing and equilibrium.
External Ear
The external ear consists of the auricle which collects the sound which then travels down the external auditory meatus.
Middle Ear
The middle ear begins with the tympanic membrane, and is an air-filled space (tympanic cavity) housing the auditory ossicles. Three auditory ossicles are the malleus, incus and stapes. The tympanic membrane vibrates the malleus, which vibrates the incus, then the stapes. The stapes vibrates the fluid inside the oval window of the inner ear. Auditory ossicles both transmit and amplify sound waves.
Auditory Tube
The auditory (eustachian) tube connects the middle ear to the throat to help maintain equal air pressure on both sides of the eardrum.
Inner Ear
The inner ear is made up of a membranouslabyrinth inside an osseous labyrinth. Between the two labyrinths is a fluid called perilymph. Endolymph is inside the membranous labyrinth. The cochlea houses the organ of hearing while semicircular canals function in equilibrium. Within the cochlea, the oval window leads to the upper compartment, called the scala vestibuli. A lower compartment, the scala tympani, leads to the round window. The cochlear duct lies between these two compartments and is separated from the scala vestibule by the vestibular membrane, and from the scala tympani by the basilar membrane. The organ of Corti, with its receptors called hair cells, lies on the basilar membrane. Hair cells possess hairs that extend into the endolymph of the cochlear duct. Above the hair cells lies the tectorial membrane, which touches the tips of the stereocilia. Vibrations in the fluid of the inner ear cause the hair cells to bend resulting in an influx of calcium ions. This causes the release of a neurotransmitter from vesicles that stimulate the ends of nearby sensory neurons.
Auditory Nerve Pathways
Nerve fibers carry impulses to the auditory cortices of the temporal lobes where they are interpreted.
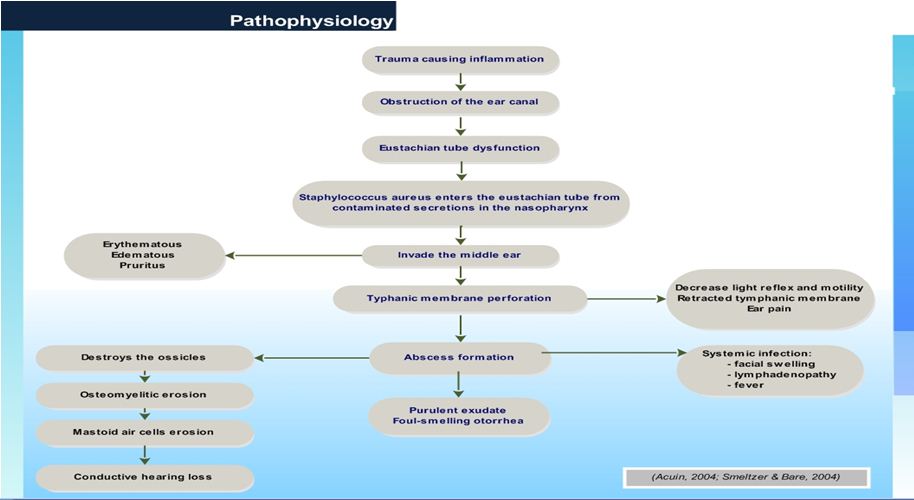
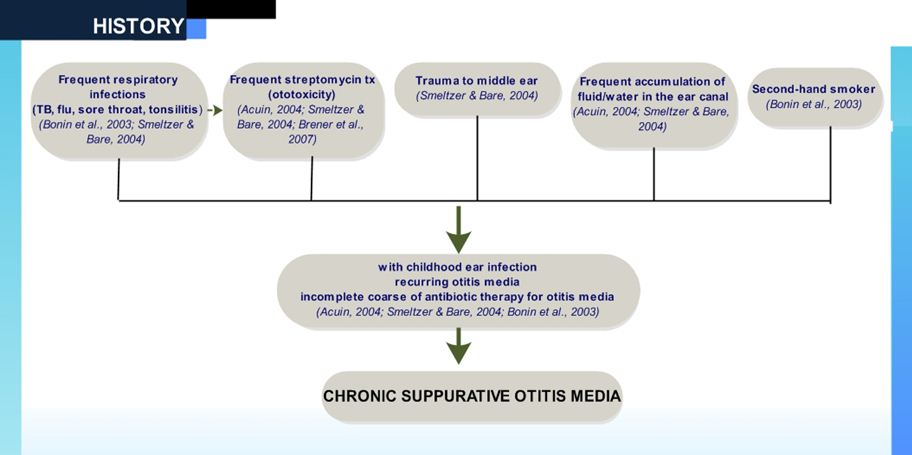
Pathophysiology
Diagnostic Examination
CBC with WBC differential count
Hemoglobin, hematocrit, and red blood cell counts may reveal normal. WBC differential count reveals elevated white blood cells, neutrophils, lymphocytes and monocytes counts that indicate severe inflammatory process and bacterial infections (McFarland & Grant, 1988).
Culture and Sensitivity Testing of discharge reveal the presence of staphylococcus aureus – one of the most common bacterial pathogens of otitis media (Smeltzer & Bare, 2004).
Staphylococcus aureus is a respiratory pathogen that may have been insufflated from the nasopharynx into the middle ear through the Eustachian tube during bouts of upper respiratory infections. The bacteria is infrequently found in the skin of the external canal, but may proliferate in the presence of trauma, inflammation, lacerations, or high humidity which may then gain entry to the middle ear through a chronic perforation (Acuin, 2004).
CT Scan revealed perforation of the tympanic membrane, ossicular abscess, and erosions of the bony partitions of the mastoid air cells. Absence or presence of cholesteatoma. Labyrinth and temporal bones may be intact or damaged.
The staphylococcus areus has infected and eroded the tympanic membrane causing perforation, ossicles and the mastoid bony partitions which may cause a conductive hearing loss. CSOM can cause chronic mastoiditis and lead to cholesteatoma formation. It can occur in the middle ear, mastoid cavity, or both. If untreated, cholesteatoma will continue to enlarge, possibly causing damage to the facial nerve and horizontal canal and destruction of other surrounding structures. The absence of cholesteatoma is a good indication that the condition is not malignant and not cancerous. Intactness of the labyrinth and temporal bones are signs that there will be no sensorineural defect (Smeltzer & Bare, 2004; Acuin, 2004).
Chronic Suppurative Otitis Media Assessment Tool and Treatment Model
Nursing Care Plan
The two major problems of chronic suppurative otitis media are infection and pain (particularly, in the presence of mastoiditis). In case of fever, infection is the underlying cause of fever—if the infection is treated, then fever will disappear.
(Doenges, M. E. et al, 2008; Gulanick, M. & Myers, J. L., 2007; Johnson, M. et al , 2007; Roth, R. A., 2007)
Other Nursing Concerns:
- Anxiety management
- Improving hearing and communication
- Promote wound healing and return of skin integrity
- Patient and significant other’s knowledge about the disease, treatment, and prevention.
- Initiating self-care and continuing care at home
Medications
Anti-infective: Ofloxacin Otic
An antibiotic of Fluoroquinolone class, which inhibits bacterial DNA gyrase and prevents DNA replication in susceptible bacteria. Kills susceptible to aerobic gram-positive and gram-negative organisms. Indication and dosage: for Chronic Suppurative Otitis Media – twice daily on the affected ear for 14 days.
Anti-infective :Amoxicillin Oral
An antibiotic of Aminopenicillin type that inhibits cell- wall synthesis during bacterial multiplication. Kills susceptible bacteria. Indication and dosage: for severe infections of the ear – 500 mg/capsule 1 capsule every 8 hrs. for 7 days.
Anti-pyretic / Analgesic : Paracetamol
Para-aminophenol derivative, which may produce an analgesic effect by blocking pain impulses, by inhibiting prostaglandin or pain receptor sensitizers. May relieve fever by acting in the hypothalamic heat-regulating center. Relieves pain and reduces fever. Indication and dosage: mild pain or fever – 500 mg/tablet 1 tablet every 4 hrs., PRN.
Pain-reliever: Mefenamic Acid
The analgesic effect of NSAIDs may result from interference with the prostaglandins involved in pain. Prostaglandins appear to sensitize pain receptors to mechanical stimulation or to other chemical mediators. NSAIDs inhibit the synthesis of prostaglandins peripherally and possibly centrally. Like salicylates, NSAIDs exert an anti-inflammatory effect that may result in part from inhibition of prostaglandin synthesis and release during inflammation. Indication and dosage: mild to moderate pain, inflammation, stiffness, swelling, or tenderness caused by trauma or inflammatory process and surgical procedures – Mefenamic Acid 500mg/tablet 1 tablet every 8 hrs. PRN (if there is pain only) on a full stomach.
Medical Management
Local treatment
Careful suctioning can be done on the affected ear under microscopic guidance performed by an experienced physician. Proper aural toilet habit and ear care. Instillation of antibiotic drops is used to treat purulent discharges. Also, systemic antibiotics may be prescribed as indicated (Smeltzer & Bare, 2004).
Surgical treatment
Surgical procedures include tympanoplasty, ossiculoplasty and mastoidectomy. The extent of damage and infection determines the type of procedure/s to be performed. Tympanoplasty is the surgical reconstruction of the tympanic membrane which requires ossicles reconstruction. This procedure restores middle ear function, close the perforation, prevent recurrent infection and improve hearing. Ossiculoplasty, surgical reconstruction of the middle ear bones to restore hearing by re-establishing the sound conduction mechanism. Mastoidectomy is done to remove the cholesteatoma, gain access to diseased structures, and create a dry and healthy ear (Smeltzer & Bare, 2004; Goldman, 1996).
Complications
Preventing injury from vertigo. Vertigo occurs if the semicircular canals or other areas of the inner ear are traumatized during mastoid surgery (Smeltzer & Bare, 2004).
Preventing altered sensory perception. Facial nerve (cranial nerve VII) injury is a potential but rare complication of mastoid surgery. Chorda tympani nerve disturbance may occur resulting to alteration in taste and dry mouth on the side of the surgery but soon will disappear until the nerve regenerates (Smeltzer & Bare, 2004).
Health Teaching
Scope
Cognitive: Be able to identify the effects and actions of every medication.Psychomotor: Patient and significant others will be able to demonstrate the proper administration of drugs (oral and otic).Affective: Be able to understand the importance of adherence to the medication regimen.
Cognitive: Patient and significant others will be able to understand the procedures in aural toilet habit.Psychomotor: Patient and significant others will be able to demonstrate the procedures of aural toilet habit.Affective: Patient and significant others will be able to understand the importance of the procedures of aural toilet habit and the importance of compliance for the early recovery of the patient.
Topics
- Administration of take home medications.a. proper time, dosage and route of administration
-
-
- importance of adherence to medications
- layman’s explanation on pharmacology and pharmacokinetics of medications
- does and don’ts when taking the medications
- proper instillation of otic drops
-
- Aural toilet habitat. Proper oral cleaning. Proper cleaning of the post-operative site
-
- Aseptic techniques in cleaning post-operative site
- Handwashing techniques
-
Evaluation
Able to identify that ofloxacin drops and amoxicillin are antibiotics that fight infection and dose should be completed to prevent the recurrence. Identify that paracetamol should only be taken every four hours if there is fever and mefenamic acid if there is pain–both should be taken on a full stomach to prevent GI ulcer. Provide written instructions to memorize the schedule of medication intake. Confidence in performing the proper instillation of otic drops. Understands the importance of full adherence to the medical regimen.
Confidence to perform proper ear cleaning, aural toilet interventions, and instillation of otic drops. The patient and significant others verbalized the importance of handwashing and aseptic techniques when handling the post-operative site. Practice handwashing and applying alcohol most of the time.
Discharge Plan
Medications: Pain-reliever, antipyretic and antibiotic medications as prescribed, with proper instructions on intake, administration, and compliance.
Environmental: Avoidance of noise-pollution and other hearing hazards. Provide sounds soothing to ears.
Treatment: Proper aural toilet habit and aseptic daily post-op wound care with proper instructions on how to perform the procedures.
Health Teaching: Improving hearing and communication techniques. Health promotion and prevention of the possible recurrence and occurrence of complications.
Out-patient: Follow up consultation after 1 week, as indicated, and or as advised. Importance of compliance with continuous care at home.
Diet: Dietary management of foods rich in protein, iron, vitamin C, and zinc. Avoid foods rich in sodium and cholesterol as it may impair tissue healing; sugar control for diabetic clients. Emphasize the importance of diet for rehabilitation and fast recovery.
Health promotion and prevention are the functions of the primary health care system. Mass awareness and education about CSOM can avert social stigma thus, promoting acceptance. This will play a vital role in screening and early detection. A history of at least 2 weeks of persistent ear discharge should alert primary health workers to the problem. Hearing loss can be prevented if people will listen and learn the ways on how it can be avoided.
CSOM may lead to hearing loss or deafness. Antibiotics and surgeries are very expensive. Its effects are not only centered on the social stigma moreover, its burden is on the permanent damage of deafness. But it can be prevented, early detection and management will save thousands of patients from deafness. Early management will save you from the expensive costs of medications, surgery, and hospitalization.
References:
- Acuin, J. (2004). Chronic Suppurative Otitis Media: Burden of Illness and Management Options. Geneva, Switzerland: World Health Organization Publication, 7–10, 20. Bonin, E. et al. (2003).
- Adapting Your Practice: Treatment and Recommendations for Homeless Children with Otitis Media. Nashville: Health Care for the Homeless Clinician’s Network, 1–3. Brener T. et al. (2007).
- Springhouse Nurse’s Drug Guide 2007, 8th ed. Philadelphia: Lippincott Williams & Wilkins, 1175, 934–937, 149–151, 99–101, 75–76. Doenges, M. E. et al. (2008).
- Nurse’s Pocket Guide: Diagnoses, Prioritized Interventions, and Rationales, 11th ed. Philadelphia: F.A. Davis Company, 409–413, 498–503.
- Goldman, M. A. (1996). Pocket Guide to the Operating Room, 2nd ed. Philadelphia: F.A. Davis Company, 437–440. Gulanick, M. & Myers, J. L. (2007). Nursing Care Plans: Nursing Diagnosis and Intervention, 6th ed. Singapore: Mosby Elsevier, 108–112, 144–149. Johnson, M. et al. (2007). NANDA, NOC, and NIC Linkages: Nursing Diagnoses, Outcomes, & Interventions, 2nd ed. Singapore: Mosby Elsevier, 557–561, 303–305. McFarland, M. B. & Grant, M. M. (1988).
- Nursing Implications of Laboratory Tests, 2nd ed. New York: Delmar Publishers, Inc., 19–30. Roth, R. A. (2007). Nutrition & Diet Therapy, 9th ed. Singapore: Delmar and Thomson Asia Pte Ltd., 382. Smeltzer, S.C. & Bare, B.G. (2004).
- Brunner & Suddarth’s Textbook of Medical-Surgical Nursing, 10th ed. PA: Lippincott Williams & Wilkins, 1802–1805. Sheir, D.N. et al (2006). Hole’s Essentials of Human Anatomy & Physiology, 9th ed. New York: McGraw-Hill Companies, Inc.








Thank you so much mam.. You r doing a gr8 job. Plz show me the path of knowledge..i m a 3rd year b.sc nursing student..uor biadata have inspired a lot.. I want to become like you .. Plzz plzz plzz show me the path.. And help me to become like you..
Sohini chandra : Thank you so much. I believe you can do better than I did. You are still young … and for sure you will be better than me in the near future. Just study hard and focus on your dreams … strive harder beyond what you can do. We always have that adrenaline power… it will be released the more you aspire … have a great day!