Introduction
The human cardiovascular system is a remarkable network of organs, blood vessels, and fluids that deliver vital oxygen and nutrients. This intricate system is crucial in maintaining overall health and well-being, from the heart to the blood vessels. Understanding the anatomy and physiology of the cardiovascular system is essential for healthcare professionals to diagnose and manage cardiovascular diseases effectively. In this article, we will delve into the cardiovascular system’s complexities, the anatomy and physiology of the heart, the intricacies of blood circulation, and the importance of maintaining cardiovascular wellness. Through extensive research and reliable sources, we aim to provide a comprehensive and up-to-date guide that educates and engages our readers on this fascinating topic.
Overview of the Article
This article is divided into three parts that provide an in-depth understanding of the cardiovascular system. The first part delves into the anatomy and physiology of the heart, highlighting the structure and function of the four chambers, the electrical conduction system, and the cardiac cycle. The second part explores blood circulation, discussing the three key areas of circulation: pulmonary, cardiac, and systemic. It also covers the crucial interplay of preload, contractility, and afterload for optimal cardiac function. The third and final part navigates blood pressure and cardiovascular wellness, emphasizing the significance of blood pressure as a cardiovascular compass and providing proactive measures to foster a robust cardiovascular system.
The Heart: The Centerpiece of the Cardiovascular System
The human heart, a muscular organ, resides within the mediastinum, nestled between the lungs in the thoracic cavity. Its conical shape is akin to the size of a clenched fist. The heart is divided into four chambers: two atria (left and right) and two ventricles (left and right). The atria collect blood returning to the heart, while the ventricles pump blood out and into circulation.
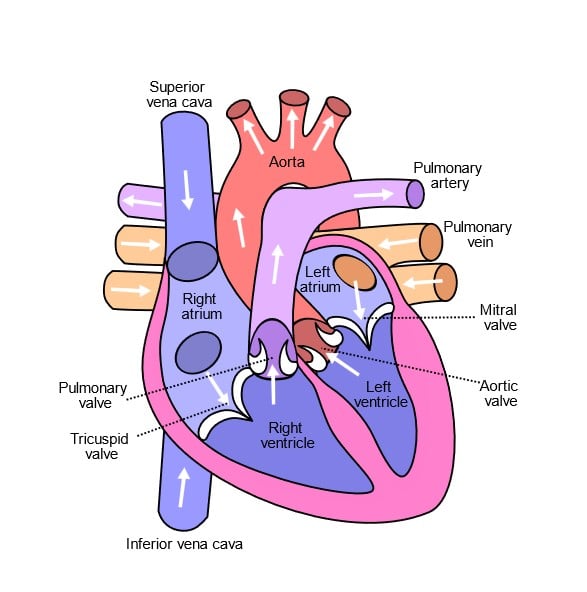
The heart’s muscular wall, the myocardium, comprises specialized cardiac muscle cells. These cells possess unique properties, such as automaticity (the ability to generate electrical impulses without external stimulation) and rhythmicity (the regularity of electrical impulse generation). The heart’s electrical system initiates and coordinates the contraction of cardiac muscle cells, ensuring efficient blood pumping.
The Heart’s Chambers: A Journey Through the Atria and Ventricles
The heart, a marvel of biological engineering, features four distinct chambers: two atria and two ventricles, each with unique function and characteristics.
Welcome to the Atria: The Upper Receiving Chambers
The atria in the heart’s upper region are separated by the interatrial septum. These chambers collect blood returning to the heart and supply it to the ventricles. Acting as the heart’s welcoming committee, the atria play a critical role in circulation.
The right atrium receives blood from the superior and inferior venae cavae, while the left atrium, smaller but boasting thicker walls, occupies the highest part of the heart’s left border. Here, the left atrium greets blood from the four pulmonary veins.
Exploring the Ventricles: The Lower Pumping Chambers
Descending into the lower chambers, the right and left ventricles are divided by the interventricular septum. These muscular chambers receive blood from the atria and pump it to the lungs and the rest of the body.
The ventricles, with their highly developed musculature, are larger and possess thicker walls than the atria, a testament to their vital role in pumping blood throughout the body.
The right ventricle diligently sends blood to the lungs. In contrast, the left ventricle, characterized by its considerably thicker wall, propels blood into the aorta, ensuring a steady supply of oxygen and nutrients to every corner of the body.
Heart Structure: A Comprehensive Overview
The heart, a vital organ for pumping blood throughout the body, boasts a complex structure that facilitates its crucial functions. Surrounded by the pericardium, a sac composed of fibrous and serous layers, the heart’s wall consists of three distinct layers: the myocardium, endocardium, and epicardium. Within the heart, four chambers—two atria and two ventricles—work in tandem with four valves—two atrioventricular (AV) and two semilunar valves—to maintain efficient blood flow.
The Protective Pericardium
The pericardium, a fibro serous sac, encloses the heart and the roots of the great vessels that enter and exit the heart. It comprises two components: the fibrous pericardium and the serous pericardium. The fibrous pericardium, a tough, white fibrous tissue, fits loosely around the heart, providing protection. Meanwhile, the serous pericardium, a thin, smooth inner layer, consists of the parietal layer that lines the fibrous pericardium’s interior and the visceral layer that adheres to the heart’s surface.
Lubricating the Pericardial Space
Between the fibrous and serous pericardium lies the pericardial space. This cavity contains pericardial fluid, which lubricates the surfaces of the space, allowing the heart to move effortlessly during contraction.
Delving into the Heart’s Wall
The heart wall is composed of three distinct layers:
- Epicardium: The outer layer, also known as the visceral layer of the serous pericardium, consists of squamous epithelial cells overlying connective tissue.
- Myocardium: The middle layer, which forms most of the heart wall, comprises striated muscle fibers that enable the heart to contract.
- Endocardium: The inner layer of the heart comprises endothelial tissue, small blood vessels, and smooth muscle bundles.
Location and Orientation of the Heart
The heart is located in the mediastinum, a cavity that houses not only the heart but also the great vessels and trachea. Positioned beneath the sternum, the heart predominantly extends to the left of the body’s midline, with nearly two-thirds of the organ near the left midclavicular line. The heart sits at an oblique angle, with its broader region, known as the base, towards the upper right side and the pointed end, referred to as the apex, towards the lower left. The apex represents the location of maximal impulse, where heart sounds are the most audible.
Blood Vessels
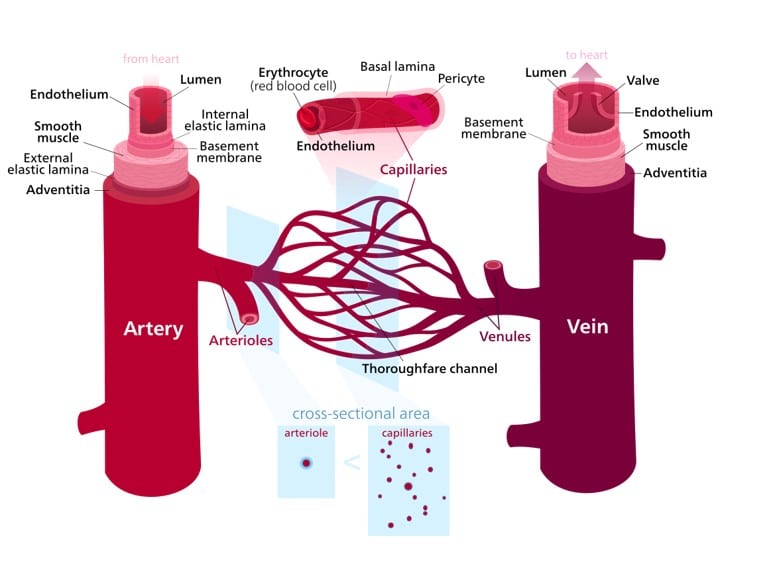
Blood vessels form an intricate network throughout the body, carrying blood to and from the heart. There are three main types of blood vessels:
- Arteries: Thick-walled vessels that transport oxygen-rich blood away from the heart, except for the pulmonary artery, which carries oxygen-poor blood to the lungs.
- Veins: Thin-walled vessels that return oxygen-poor blood to the heart, except for the pulmonary veins, which carry oxygen-rich blood from the lungs.
- Capillaries: The smallest blood vessels, connecting arteries and veins, where the exchange of oxygen, nutrients, and waste occurs between blood and tissues.
Physiology of the Cardiovascular System
The cardiovascular system operates through two primary circulatory loops: systemic circulation and pulmonary circulation. Each loop serves a specific purpose in delivering and exchanging oxygen and nutrients, ensuring the efficient functioning of our body’s cells and organs.
Systemic Circulation: The Journey of Oxygen-Rich Blood
Systemic circulation involves transporting oxygen-rich blood from the heart to the body’s cells and tissues. The process begins when the left ventricle pumps blood into the aorta, which then distributes it to the rest of the body through a network of branching arteries. As blood travels through the systemic circulation, oxygen and nutrients are delivered to cells. In turn, oxygen-poor blood laden with waste products is collected by veins, which converge into the superior and inferior vena cava. This deoxygenated blood returns to the right atrium, completing the systemic circulation loop.
Pulmonary Circulation: The Exchange of Gases in the Lungs
Pulmonary circulation replenishes the blood’s oxygen content while removing carbon dioxide. Oxygen-poor blood from the right atrium flows into the right ventricle, which pumps it into the pulmonary artery. The pulmonary artery transports the blood to the lungs, where essential gas exchange occurs within the alveoli. Oxygen from the inhaled air diffuses into the bloodstream, while carbon dioxide is expelled from the blood into the air during exhalation. Following this exchange, oxygen-rich blood returns to the left atrium via the pulmonary veins, ready to be distributed throughout the body once more.
The intricate and harmonious interplay between systemic and pulmonary circulation loops underpins the efficient functioning of the cardiovascular system. Understanding these processes is crucial for maintaining overall health and well-being. The cardiovascular system is pivotal in delivering oxygen and nutrients and removing waste products from the body.
Branching Pathways: Delivering Lifeblood to the Body
The aorta, the body’s largest artery, branches off into many smaller vessels that supply specific organs and areas of the body. As the aorta emerges from the heart and extends downward, key arteries branch off to ensure the upper body receives an adequate blood supply:
- The left common carotid artery supplies blood to the brain.
- The left subclavian artery delivers blood to the arms.
- The brachiocephalic artery ensures the upper chest receives blood.
As the aorta descends through the thorax and abdomen, its branches supply the gastrointestinal and genitourinary systems, spinal column, and chest and abdominal muscles. Finally, the aorta divides into the iliac arteries, which further branch into femoral arteries, providing blood to the lower limbs.
Division and Dilation: Expanding the Area of Perfusion
Arteries divide into smaller units, dramatically increasing the number of vessels and the area of tissue receiving blood flow, also known as perfusion. Sphincters control blood flow into tissues at the junction of arterioles and capillaries, dilating to allow increased flow when needed or constricting to reduce blood flow.
A Vast Network of Low-Pressure Capillaries
Despite containing the smallest vessels, the capillary bed supplies blood to the largest number of cells, facilitating the exchange of nutrients, oxygen, and carbon dioxide with body cells. Capillary pressure is low to enable this exchange, and blood flows from capillaries into venules and eventually into veins.
One-Way Traffic: Preventing Blood Backflow
Valves in veins prevent blood backflow, and pooled blood in each valved segment is moved toward the heart by pressure from the moving volume of blood below. Veins merge to form two main branches, the superior and inferior vena cava, which return blood to the right atrium.
Coronary Circulation: Nourishing the Heart
The heart relies on coronary arteries and their branches to supply oxygenated blood and depends on cardiac veins to remove deoxygenated blood. During diastole, blood flows out of the heart into the aorta and coronary arteries, nourishing the heart.
Age-Related Cardiovascular Changes
As a normal part of aging, the heart becomes slightly smaller, and its contractile strength declines, reducing efficiency. Resting cardiac output typically diminishes 30% to 35% by age 70. Veins dilate and stretch, coronary artery blood flow drops, and the aorta becomes more rigid, resulting in a widened pulse pressure. Left ventricular walls grow thicker, and heart valves thicken due to fibrotic and sclerotic changes, which may cause systolic murmurs.
The Cardiac Cycle: Diastole and Systole Explained
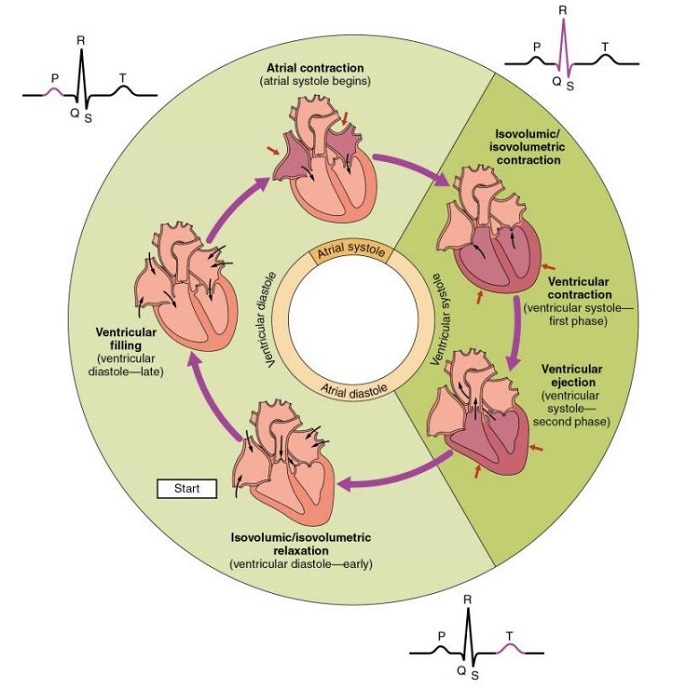
OpenStax, Phases of the Cardiac Cycle.
https://commons.wikimedia.org/wiki/File:2027_Phases_of_the_Cardiac_Cycle.jpg
The cardiac cycle is a complex process that consists of two primary phases: diastole and systole. Diastole is characterized by the heart chambers’ relaxation and subsequent filling with blood. In contrast, systole involves the contraction of these chambers and the ejection of blood from the heart. The heart’s electrical system coordinates these events, including the sinoatrial (SA) node, atrioventricular (AV) node, and the bundle of His and Purkinje fibers.
The sinoatrial (SA) node, commonly known as the heart’s natural pacemaker, initiates electrical impulses that cause the atria to contract. The atrioventricular (AV) node receives these impulses and temporarily delays them, ensuring the ventricles have sufficient time to fill with blood. Following this brief pause, the bundle of His and Purkinje fibers convey the impulses to the ventricles, prompting them to contract and propel blood to the lungs and the rest of the body.
The Heart’s Electrical Conduction System: A Vital Component
The heart’s electrical conduction system plays a crucial role in synchronizing the contraction and relaxation of the heart chambers. The sinoatrial (SA) node generates electrical impulses that instigate the contraction of the atria. These impulses then progress to the atrioventricular (AV) node, where they are momentarily delayed, allowing the ventricles to fill with blood before contracting.
After the delay at the AV node, the impulses proceed to the bundle of His, which bifurcates into the left and right bundle branches. These branches further subdivide into the Purkinje fibers, responsible for dispersing the electrical impulses across the ventricular walls. Consequently, the ventricles contract and pump blood to the lungs and the rest of the body.
Blood Circulation and Oxygen Delivery: The Cornerstone of Cellular Health
As the ventricles contract, they direct blood to different body regions. The right ventricle pumps deoxygenated blood to the lungs, acquiring oxygen. Conversely, the left ventricle expels oxygen-rich blood to the rest of the body, ensuring the efficient delivery of oxygen and essential nutrients to every cell.
The well-coordinated and effective nature of this process is vital for sustaining the overall health and function of the body. Cells rely on a consistent supply of oxygen and nutrients to function optimally. The harmonious operation of the cardiac cycle and the cardiovascular system plays a pivotal role in ensuring these needs are consistently met.
By delving into the complexities of the cardiac cycle and comprehending the significance of blood circulation, we can better appreciate the vital function of the cardiovascular system in maintaining our overall health and well-being.
Exploring Cardiac Output and Blood Flow Dynamics
Cardiac Output: The Heart’s Masterful Performance
Cardiac output is a crucial measure of the heart’s efficiency, representing the volume of blood pumped by the heart within a minute. This value is determined by the heart rate and stroke volume, which is the quantity of blood ejected during each heartbeat.
The stroke volume is influenced by three primary factors: preload, contractility, and afterload. These elements work in harmony to modulate the heart’s pumping capacity, ensuring the optimal distribution of blood to meet the body’s ever-changing needs.
The Journey of Blood Flow: A Tale of Three Circuits
Blood embarks on an intricate voyage through the vascular system, traversing three distinct types of blood vessels and navigating three key areas of circulation: pulmonary, cardiac, and systemic.
In the pulmonary circuit, blood is oxygenated as it journeys through the lungs, while the cardiac circuit supplies the heart muscle with life-giving oxygen and nutrients. Lastly, the systemic circuit delivers vital oxygen and nutrients to all other tissues and organs throughout the body.
Balancing the Pump: The Crucial Interplay of Preload, Contractility, and Afterload for Optimal Cardiac Function
Preload: The Foundation for Adequate Ventricular Filling
Preload refers to the extent of stretching experienced by ventricular muscle fibers due to the blood volume in the ventricles at the end of diastole. This stretching is critical for optimal ventricular filling, directly impacting the heart’s pumping efficiency.
Contractility: The Inherent Force of Cardiac Muscle Contraction
Contractility signifies the intrinsic capacity of the heart muscles to contract effectively. This property is directly influenced by preload, as a greater stretch of the muscle fibers leads to more forceful contractions, known as the Frank-Starling mechanism. Consequently, contractility is vital in determining the heart’s ability to pump blood throughout the body.
Afterload: The Pressure Challenge for Ventricular Ejection
Afterload represents the pressure that ventricular muscles must generate to overcome resistance in the aorta and pulmonary arteries, ensuring blood is efficiently ejected from the heart. An increase in afterload can decrease stroke volume, which is the volume of blood ejected from the heart during a single beat. Maintaining an appropriate afterload is crucial for ensuring the heart’s efficient performance.
Blood Pressure as a Cardiovascular Compass
Blood pressure, the force exerted by the blood upon the walls of blood vessels, is a vital gauge of cardiovascular health. Intricately regulated by factors such as cardiac output, peripheral resistance, and blood volume, an equilibrium among these elements ensures the sufficient perfusion of organs and tissues, thereby safeguarding cardiovascular well-being.
Charting the Course to Cardiovascular Vitality
Recognizing and preserving cardiovascular health is paramount for overall well-being. Embrace the following proactive measures to foster a robust cardiovascular system:
- Energize Your Heart: Regular physical activity, such as 150 minutes of moderate-intensity aerobic exercise per week, bolsters cardiovascular health, reduces blood pressure and minimizes the risk of heart disease.
2. Savor a Heart-Healthy Diet: A nourishing diet abundant in fruits, vegetables, whole grains, lean proteins, and healthy fats promotes proper weight, cholesterol levels, and blood pressure, mitigating the risk of cardiovascular disease.
3. Extinguish Tobacco’s Grip: Smoking is a formidable risk factor for cardiovascular disease. Ceasing tobacco use significantly diminishes the risk of heart attack, stroke, and other heart-related complications.
4. Master the Art of Stress Management: Chronic stress can contribute to high blood pressure and other cardiovascular issues. Cultivating stress management techniques such as meditation, deep breathing, and regular exercise can help maintain a healthy heart.
5. Embrace Routine Check-ups: Regular medical examinations and screenings can identify potential risk factors and enable early intervention, reducing the risk of cardiovascular disease.
Concluding the Cardiovascular Journey
The heart pumps life-sustaining blood to every corner of our body, a feat the complex and intricate cardiovascular system makes possible. This system is a web of organs, vessels, and fluids that harmonize to deliver vital oxygen and nutrients throughout our bodies. From the heart’s four chambers to the cardiac cycle’s intricate sequence of events, this guide explores the cardiovascular system’s fascinating anatomy and physiology.
As blood flows through the body, it delivers oxygen and nutrients to cells while collecting waste products. The harmonious operation of the cardiac cycle and the cardiovascular system is crucial to ensuring cells receive consistent oxygen and nutrients. Factors such as cardiac output, peripheral resistance, and blood volume regulate blood pressure, which is a vital gauge of cardiovascular health. Understanding these essential components can help healthcare professionals diagnose and manage cardiovascular diseases effectively.
To maintain a healthy heart, proactive measures such as regular physical activity, a heart-healthy diet, cessation of tobacco use, stress management, and routine medical examinations are crucial. This guide serves as a comprehensive and up-to-date resource on the cardiovascular system, providing insights into the system’s intricate workings and the measures we can take to ensure its optimal function.
References
- American Heart Association. (2021). Heart Disease and Stroke Statistics-2021 Update. Circulation, 143(8). https://doi.org/10.1161/CIR.0000000000000757
- Centers for Disease Control and Prevention. (2020). Smoking and Heart Disease and Stroke. Retrieved from https://www.cdc.gov/tobacco/campaign/tips/diseases/heart-disease-stroke.html
- Granger, C. B., & Armstrong, P. W. (2015). Preload and afterload in clinical cardiology. In Hurst’s the heart (pp. 99-107). McGraw-Hill Education.
- Guyton, A. C., & Hall, J. E. (2016). Textbook of Medical Physiology (13th ed.). Elsevier. https://www.elsevier.com/books/guyton-and-hall-textbook-of-medical-physiology/guyton/978-1-4557-7005-2
- Jorde, U. P., Kushwaha, S. S., Tatooles, A. J., Naka, Y., Bhat, G., Long, J. W., … & Stehlik, J. (2018). Results of the destination therapy post-food and drug administration approval study with a continuous flow left ventricular assist device: a prospective study using the INTERMACS registry (Interagency Registry for Mechanically Assisted Circulatory Support). Journal of the American College of Cardiology, 71(12), 1397-1409.
- Klabunde, R. E. (2019). Cardiovascular Physiology Concepts. Lippincott Williams & Wilkins.
- Maeder, M. T., & Kaye, D. M. (2018). Understanding preload reserve and afterload mismatch in the failing heart. Heart Failure Reviews, 23(3), 289-300.
- Marieb, E. N., & Hoehn, K. (2018). Human Anatomy & Physiology (11th ed.). Pearson. https://www.pearson.com/us/higher-education/program/Marieb-Human-Anatomy-Physiology-11th-Edition/PGM334540.html
- OpenStax College. (n.d.). Phases of the Cardiac Cycle. https://commons.wikimedia.org/wiki/File:2027_Phases_of_the_Cardiac_Cycle.jpg, CC by 3.0
- Patton, K. T., & Thibodeau, G. A. (2019). Anatomy & physiology. Mosby.
- Perry, A. G., Potter, P. A., & Desmarais, P. L. (2019). Mosby’s pocket guide to nursing skills & procedures. Elsevier.
- Ponikowski, P., Voors, A. A., Anker, S. D., Bueno, H., Cleland, J. G. F., Coats, A. J. S., … & Jessup, M. (2018). 2016 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure: The Task Force for the diagnosis and treatment of acute and chronic heart failure of the European Society of Cardiology (ESC) Developed with the special contribution of the Heart Failure Association (HFA) of the ESC. European Heart Journal, 37(27), 2129-2200.
- Saladin, K. S. (2018). Anatomy & Physiology: The Unity of Form and Function (8th ed.). McGraw-Hill Education. https://www.mheducation.com/highered/product/anatomy-physiology-unity-form-function-saladin/M9781259277726.html
- Silverthorn, D. U. (2020). Human Physiology: An Integrated Approach (8th ed.). Pearson. https://www.pearson.com/us/higher-education/program/Silverthorn-Human-Physiology-An-Integrated-Approach-Plus-Mastering-A-P-with-Pearson-e-Text-Access-Card-Package-8th-Edition/PGM335152.html
- Tortora, G. J., & Derrickson, B. H. (2017). Principles of Anatomy and Physiology (15th ed.). Wiley. https://www.wiley.com/en-us/Principles+of+Anatomy+and+Physiology%2C+15th+Edition-p-9781119329398
- Widmer, R. J., & Lerman, A. (2018). Endothelial dysfunction and cardiovascular disease. Global Cardiology Science and Practice, 2018(3), e201811.
- World Health Organization. (2021). Cardiovascular diseases (CVDs). Retrieved from https://www.who.int/news-room/fact-sheets/detail/cardiovascular-diseases-(cvds)