The urinary system plays a crucial role in ensuring our well-being and operates silently behind the scenes. Its primary objective is to regulate the blood’s composition and volume by eliminating excess fluid and waste products from the body.This system comprises two kidneys, two ureters, a urinary bladder, and a urethra responsible for filtering our blood, maintaining electrolyte balance, and eliminating waste materials. In this comprehensive guide, we will delve into the captivating universe of urinary system anatomy and physiology while also examining conventional illnesses that can affect us adversely. This information is of immense value for nurses, students pursuing healthcare education, and individuals seeking to comprehend the importance of this critical physiological mechanism.
A Guided Tour of the Urinary System: An In-Depth Exploration
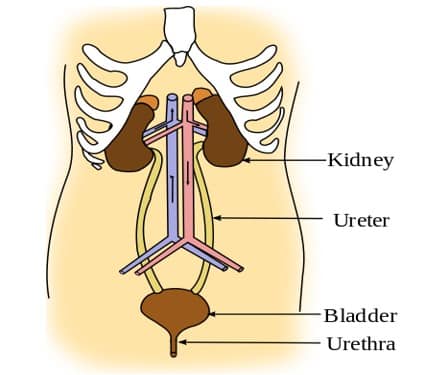
Kidneys: These bean-shaped organs, located on either side of the spine, are the superstars of the urinary system. They filter our blood to remove waste products and excess fluids, transforming them into urine. Each kidney contains approximately one million filtering units called nephrons, which are responsible for filtering waste and regulating electrolyte levels. The nephron is the basic functioning unit of the kidney, consisting of a glomerulus, which is a network of capillaries located within a structure called Bowman’s capsule, and a series of complicated twisted tubules.
Ureters: These muscular tubes, measuring around 10-12 inches in length, act as highways, transporting urine from the kidneys to the bladder via peristaltic contractions. The ureters’ precise coordination prevents urine backflow, safeguarding the kidneys from potential damage.
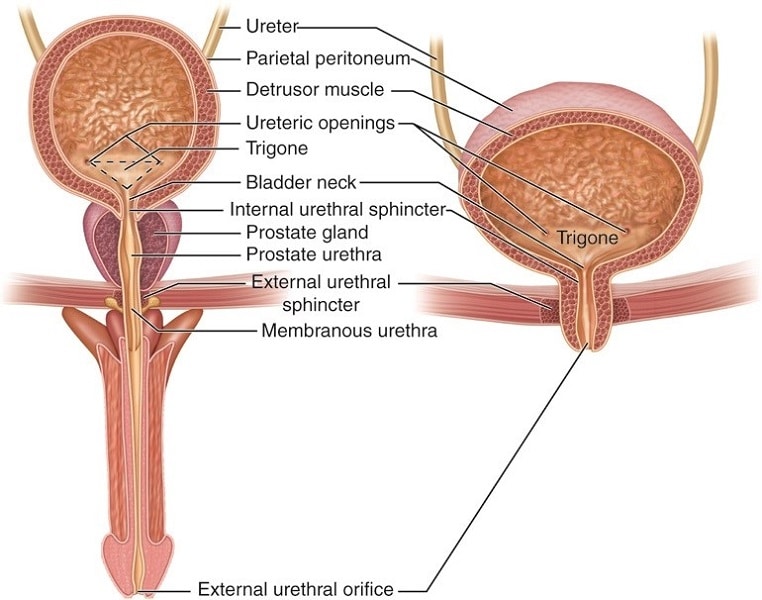
Bladder: This muscular, balloon-like organ is situated in the pelvic cavity and stores urine until we’re ready to expel it from our body. The bladder can hold between 300-500 milliliters of urine before the urge to urinate arises. The detrusor muscle, which lines the bladder, and the internal and external urethral sphincters work in harmony to enable seamless urine storage and release.
Urethra: This canal serves as the final exit for urine, guiding it out of the body during urination. The urethra’s length and function differ between males and females. In males, it is longer and transports both urine and semen, while in females, it is shorter and solely responsible for urine elimination.
Mastering the Urinary System: The Physiology of the Urinary System: Achieving Perfect Balance
Kidneys: The Guardians of Homeostasis
The kidneys serve as the body’s homeostasis champions, skillfully maintaining the delicate equilibrium of water, electrolytes, and pH levels. They also generate crucial hormones such as erythropoietin for red blood cell production and renin for blood pressure regulation. Furthermore, kidneys activate vitamin D, which is essential for bone health.
Regulating Blood Pressure and Composition
The urinary system’s functions extend beyond waste removal. The kidneys continuously monitor and adjust blood pressure, playing a pivotal role in maintaining optimal levels. In addition, the urinary system ensures a balance between water and electrolyte concentrations, regulating blood volume and composition.
Nephrons: The Fundamental Balance Keepers
The nephron, the kidney’s basic functional unit, comprises a glomerulus and a series of tubules. The glomerulus is a network of capillaries within Bowman’s capsule where filtration occurs. This process results in filtrate formation, which becomes urine after traveling through the tubules. The urine then exits the kidney via the ureters, which transport it to the bladder for storage until elimination through the urethra.
Aging and the Urinary System: Changing Dynamics
The urinary system is substantially affected by the process of aging. The count of effective nephrons reduces with age, leading to less efficient filtration and elimination of waste. Additionally, loss of muscle tone in the bladder can reduce its capacity which then leads to frequent urination. For biological males, an enlarged prostate gland narrows down the urethra which makes it challenging to empty the entire bladder resulting in urine leakage between bathroom visits. Furthermore, older individuals are at higher risk of developing urinary tract infections due to incomplete emptying of the bladder and an increased growth rate for bacteria.
Maintaining Harmony: Hydration and Kidney Health
Drinking sufficient fluids is crucial, particularly for the elderly, to maintain proper kidney function and prevent urinary tract infections. The urinary system comprises the kidneys, bladder, urethra, and ureters and plays a significant role in eliminating waste from the body while regulating fluid balance, electrolyte levels, as well as blood pressure. To summarize, adequate hydration is essential for maintaining optimal functioning of the urinary system.
Anatomy and Physiology of the Urinary System: Delving Deeper
Micturition Reflex: A Synchronized Collaboration
The intricate process of urination, also known as micturition, involves a complex interplay between the nervous system and the urinary system. When the bladder fills up with urine nearing its storage capacity, stretch receptors in the bladder wall are activated and send signals to the brain which triggers the micturition reflex. This reflex induces contraction of the detrusor muscle and relaxation of the internal urethral sphincter resulting in urine flowing into the urethra. The external urethral sphincter can be voluntarily controlled and relaxed by an individual for eliminating urine from their body.
Renal Blood Flow and Glomerular Filtration
The proper functioning of the kidneys is dependent on sufficient renal blood flow. The renal artery is responsible for transporting blood into the kidneys, dividing it into smaller arteries and arterioles before eventually forming glomerular capillaries. Filtration in the glomerulus marks the initial step in urine production through which blood plasma is passed via to Bowman’s capsule to form filtrate. This filtration process necessitates close regulation to achieve an appropriate balance of solutes and water within the body.
Tubular Reabsorption and Secretion
Following the process of glomerular filtration, the filtrate is directed toward renal tubules where secretion and reabsorption processes take place. Vital substances like glucose, electrolytes, and amino acids are selectively transferred from the tubular lumen back into the bloodstream in a phenomenon called tubular reabsorption. In contrast to this, during the process of tubular secretion, excess, and waste products present in the blood are removed and secreted into the tubular lumen for eventual excretion through urine.
Countercurrent Mechanism and Urine Concentration
The loop of Henle’s countercurrent mechanism is essential for maintaining water conservation and urine concentration in the body. This process relies on interactions between the ascending and descending limbs of the nephron, which generate a gradient in the renal medulla. As a consequence of this gradient, both passive and active reabsorption of solutes and water take place, leading to concentrated urine.
Hormonal Regulation of the Urinary System
The urinary system is regulated by several hormones, including antidiuretic hormone (ADH), aldosterone, and atrial natriuretic peptide (ANP). ADH, which is produced by the posterior pituitary gland, increases the collecting ducts’ water reabsorption. This decreases urine output and helps in keeping a balance of water in the body. Aldosterone is produced by the adrenal cortex and assists in maintaining electrolyte balance and regulating blood volume through sodium reabsorption increase and potassium secretion in distal tubules. ANP is discharged from the heart’s atria; it encourages the excretion of both sodium & water to reduce blood volume and normalize pressure. The counteraction of ADH & aldosterone results in this.
Urinary System Functions: The Balancing Act of the Body
Urinary System Functions: The body’s equilibrium is maintained by the urinary system which regulates blood volume and composition. In this section, we’ll explore the essential roles performed by the urinary system in promoting overall well-being.
Waste Removal: The Cleansing Power of Kidneys
The kidneys play a crucial role in eliminating waste substances from the bloodstream, such as urea and ammonia, by filtering them out. These byproducts are created during the metabolic process and have to be removed from the body to avoid any harmful effects. To achieve this, the kidneys produce urine that carries these toxins and is eventually eliminated from the system.
Fluid Balance: Regulating the Body’s Hydration
Maintaining the body’s fluid balance is critical, and this is where the urinary system plays a crucial role. The kidneys have the task of regulating water levels within the body by either reabsorbing it into the bloodstream or eliminating it as urine. Through this process, dehydration, fluid overload, and swelling in different areas of the body can be avoided.
Electrolyte Regulation: Keeping Minerals in Check
The regulation of electrolyte levels like sodium, potassium, and calcium is a vital function carried out by the kidneys. These minerals are crucial for various body processes such as muscle contraction, nerve impulse transmission, and sustaining a normal heartbeat. Depending on the requirements of the body, the kidneys either retain or eliminate these minerals to sustain an optimal balance in the system.
Blood Pressure Maintenance: A Fine-Tuned System
The urinary system is responsible for regulating the fluid and electrolyte levels in the blood, hence playing a vital role in maintaining appropriate blood pressure. Hormones like renin and angiotensin are produced by the kidneys that contract blood vessels while retaining water and sodium to maintain stable blood pressure levels. This process exhibits how finely-tuned the urinary system is.
Acid-Base Balance: Ensuring Optimal pH
To maintain the body’s acid-base equilibrium, the kidneys eliminate or retain hydrogen ions and bicarbonate ions. This guarantees that the blood pH remains stable, avoiding harm to cells and organs.
Unlock the Secrets to a Healthy Urinary System: Simple Habits for Optimal Function and Well-Being
To ensure a well-functioning urinary system, certain lifestyle habits, and practices must be adopted. Among these practices are:
Staying hydrated: Ensuring that you consume sufficient water can aid in the removal of waste materials from your kidneys and inhibit the development of kidney stones. Additionally, it serves to weaken urine consistency and diminishes the chances of getting urinary tract infections. It is recommended that you aim for a minimum of eight glasses daily or adhere to your healthcare provider’s guidance.
Eating a balanced diet: Opting for a diet that contains a generous amount of fresh fruits, vegetables, whole grains, low-fat proteins, and beneficial fats may aid in promoting both kidney function and holistic wellness. Furthermore, curtailing the consumption of sodium-infused food and processed meals could be instrumental in sustaining normal blood pressure rates while alleviating the burden on the kidneys.
Regular exercise: Regularly participating in physical activities can assist in managing blood pressure, regulating glucose levels within the bloodstream, and keeping a healthy weight. All of these factors are advantageous for maintaining optimal kidney health.
Limiting alcohol and caffeine intake: It’s advised to limit your alcohol and caffeine intake as they can overwork the kidneys and bladder. Choosing non-caffeinated drinks like herbal tea or water is recommended to maintain moderate consumption levels.
Practicing good hygiene: Urinary tract infections can be prevented with good hygiene practices. Women can reduce the risk of bacterial entry into the urethra by wiping from front to back after using the toilet. Both men and women should make it a habit to clean their genital area daily and urinate immediately after sexual activity in order to prevent infections.
Monitoring medication use: Frequent or excessive use of certain drugs like nonsteroidal anti-inflammatory drugs (NSAIDs) can pose a threat to the kidneys. Hence, it is advised to adhere to the suggestions of your healthcare provider and inquire about any probable impacts of medicines on your kidney function.
Regular check-ups: It is recommended to undergo routine medical check-ups in order to promptly identify any urinary system problems and launch early treatment or intervention. Remember to talk about any worrying symptoms or issues with your healthcare professional.
You can enhance your urinary system’s performance and promote better health by incorporating these healthy habits and practices into your lifestyle. Keep in mind that the proper functioning of the urinary system is critical to eliminate waste, maintaining fluid balance, regulating electrolytes, and sustaining blood pressure. Therefore, it is vital to prioritize this aspect for overall well-being.
The Power of Prevention: Warding Off Urinary System Disorders
It is important to not only incorporate healthy practices that enable your urinary system to function at its best but also recognize and tackle potential risk factors associated with prevalent urinary system disorders. Through the implementation of proactive measures, it becomes possible to minimize the likelihood of encountering complications while maintaining optimal health within your urinary system.
Preventing Kidney Stones: Solid mineral deposits known as Kidney stones can be formed in the kidneys when waste products collect and crystallize. To decrease the chances of developing this condition, it is recommended to keep yourself properly hydrated, restrict your intake of foods containing oxalate (like beetroot, rhubarb, and spinach), and minimize salt consumption.
Reducing Urinary Tract Infections (UTIs): According to Foxman (2019), UTIs refer to bacterial infections that have the potential of affecting any area of the urinary system. To prevent these infections, it is recommended to maintain hygiene standards, stay hydrated by drinking fluids, avoid using harsh types of soap or bubble baths, and opt for breathable cotton underwear.
Managing Overactive Bladder (OAB): a condition marked by sudden and involuntary urges to urinate. In order to reduce the likelihood of developing OAB, it is recommended to engage in bladder training exercises, maintain a healthy weight, stay away from irritants that can affect the bladder (like alcohol and caffeine), and perform pelvic floor exercises aimed at strengthening the muscles responsible for controlling urination.
Keeping Interstitial Cystitis (IC) at Bay: A condition is known as IC, which affects the bladder and causes persistent pain along with a frequent urge to urinate, is considered chronic. While the root cause of this ailment remains uncertain, effective management involves stress reduction techniques, staying away from potential triggers (such as spicy foods or acidic drinks), and adhering to a well-balanced diet that may help in preventing exacerbations.
Preventing Benign Prostatic Hyperplasia (BPH): BPH refers to the non-cancerous swelling of the prostate gland found in biological males, which can result in urinary problems. By keeping a healthy weight, engaging in regular exercise, and restricting consumption of caffeine and alcohol, one may decrease their chances of BPH occurrence.
It is critical to be proactive in order to keep your urinary system functioning properly and your disorders at bay. Prioritizing prevention measures, living a healthy lifestyle, and staying informed about risks and symptoms are all important aspects of protecting your urinary system and promoting overall wellness.
Urinary System NCLEX Mastery: Conquering Anatomy & Physiology Questions
- A nurse is educating a patient on the primary function of the kidneys. Which of the following statements best describes this function?
A) Production of erythropoietin
B) Regulation of blood pressure
C) Filtration of blood and formation of urine
D) Activation of vitamin D
Answer: C) Filtration of blood and formation of urine
Rationale: The primary function of the kidneys is to filter blood and form urine, effectively eliminating waste products and excess fluids from the body. While the kidneys also produce hormones, regulate blood pressure, and activate vitamin D, these are secondary functions.
- A patient is experiencing difficulty urinating due to an enlarged prostate gland. Which part of the urinary system is most likely affected by this condition?
A) Ureters
B) Bladder
C) Urethra
D) Kidneys
Answer: C) Urethra
Rationale: In biological males, the urethra passes through the prostate gland. An enlarged prostate gland can cause compression or narrowing of the urethra, making it difficult to empty the bladder completely during urination.
- A nurse is explaining the micturition reflex to a patient. Which of the following events occurs first during this reflex?
A) Contraction of the detrusor muscle
B) Relaxation of the internal urethral sphincter
C) Relaxation of the external urethral sphincter
D) Activation of stretch receptors in the bladder wall
Answer: D) Activation of stretch receptors in the bladder wall
Rationale: The micturition reflex is initiated by the activation of stretch receptors in the bladder wall as the bladder fills with urine. This event occurs before the contraction of the detrusor muscle and the relaxation of the internal and external urethral sphincters.
- Which of the following hormones is produced by the posterior pituitary gland and increases water reabsorption in the collecting ducts?
A) Aldosterone
B) Atrial natriuretic peptide (ANP)
C) Antidiuretic hormone (ADH)
D) Renin
Answer: C) Antidiuretic hormone (ADH)
Rationale: ADH is produced by the posterior pituitary gland and increases water reabsorption in the collecting ducts, reducing urine output and conserving water. Aldosterone, ANP, and renin are also involved in the regulation of the urinary system, but they serve different functions.
- The countercurrent mechanism in the loop of Henle primarily serves which of the following functions?
A) Filtration of blood plasma
B) Reabsorption of glucose and amino acids
C) Concentration of urine
D) Secretion of waste products
Answer: C) Concentration of urine
Rationale: The countercurrent mechanism in the loop of Henle plays a crucial role in concentrating urine and conserving water in the body. It involves the interaction of the ascending and descending limbs of the loop, creating a concentration gradient in the renal medulla that enables the reabsorption of water and solutes.
- Which of the following is the primary function of the nephrons in the kidneys?
A) Producing hormones
B) Activating vitamin D
C) Filtering blood and regulating electrolyte levels
D) Storing urine
Answer: C) Filtering blood and regulating electrolyte levels
Rationale: Nephrons are the basic functioning units of the kidneys, responsible for filtering blood and regulating electrolyte levels. They contain a glomerulus and a series of tubules that facilitate the filtration, reabsorption, and secretion processes required for urine formation.
- A nurse is providing education to a group of patients regarding the hormonal regulation of the urinary system. The nurse explains that one hormone counteracts the effects of antidiuretic hormone (ADH) and aldosterone to reduce blood volume and pressure. Which hormone is the nurse referring to?
A) Insulin
B) Glucagon
C) Atrial natriuretic peptide (ANP)
D) Thyroxine
Answer: C. Atrial natriuretic peptide (ANP)
Rationale: Atrial natriuretic peptide (ANP) is a hormone released by the heart’s atria that promotes sodium and water excretion, counteracting the effects of ADH and aldosterone to reduce blood volume and pressure (Gauer & Gauer, 2019). Insulin and glucagon are involved in blood glucose regulation, while thyroxine regulates metabolism.
- Which of the following processes is primarily responsible for the selective transfer of essential substances, such as glucose, amino acids, and electrolytes, from the tubular lumen back into the bloodstream?
A) Glomerular filtration
B) Tubular reabsorption
C) Tubular secretion
D) Countercurrent mechanism
Answer: B) Tubular reabsorption
Rationale: Tubular reabsorption is the process in which essential substances like glucose, amino acids, and electrolytes are selectively transferred from the tubular lumen back into the bloodstream. This process ensures that these vital substances are not lost during urine formation.
- An elderly patient is experiencing an increased frequency of urination. Which of the following age-related changes in the urinary system is most likely contributing to this issue?
A) Decreased number of functioning nephrons
B) Enlarged prostate gland
C) Reduced bladder capacity due to muscle tone loss
D) Increased risk of urinary tract infections
Answer: C) Reduced bladder capacity due to muscle tone loss
Rationale: Aging can significantly impact the urinary system. Muscle tone loss in the bladder can reduce its capacity, resulting in an increased frequency of urination. While other age-related changes, such as a decreased number of functioning nephrons, an enlarged prostate gland, and an increased risk of urinary tract infections, can also affect urinary function, they do not directly contribute to an increased frequency of urination.
- A nurse is explaining the importance of proper hydration to a patient. Which of the following statements best describes the primary benefit of adequate fluid intake for urinary system health?
A) Preventing kidney stones
B) Supporting proper kidney function
C) Reducing the risk of urinary tract infections
D) Maintaining electrolyte balance
Answer: B) Supporting proper kidney function
Rationale: Adequate fluid intake is essential for supporting proper kidney function, as it helps the kidneys effectively filter blood and form urine. While proper hydration can also prevent kidney stones, reduce the risk of urinary tract infections, and maintain electrolyte balance, these are secondary benefits compared to supporting proper kidney function.
References
- Abrams, P., et al. (2020). The Overactive Bladder: Prevalence, Societal Impact, and Treatment. European Urology, 77(3), 327-336.
- Alhazmi, H. (2020). Nephron function in the kidney: Structure, cell types, and physiological processes. Saudi Journal of Biological Sciences, 27(12), 3214-3219.
- Alsady, M., et al. (2019). The role of the Loop of Henle in urine concentration and volume regulation. American Journal of Physiology-Renal Physiology, 317(6), F1562-F1564.
- Brenner, B. M., & Rector, F. C. (2019). Brenner and Rector’s The Kidney, 11th edition. Elsevier.
- Davies, J. A. (2019). Kidney development and fetal programming. Nephron, 139(2), 124-129.
- Ferroni, M., & Taylor, A. (2020). Prevention of Urinary Tract Infections: Lifestyle and Dietary Factors. Journal of Clinical Medicine, 9(8), 2530.
- Foxman, B. (2019). The epidemiology of urinary tract infection. Nature Reviews Urology, 7(12), 653-660.
- Gauer, R., & Gauer, J. (2019). Physiology, Antidiuretic Hormone (Vasopressin). StatPearls Publishing.
- Gormley, E. A., et al. (2019). Diagnosis and treatment of overactive bladder (non-neurogenic) in adults: AUA/SUFU guideline. Journal of Urology, 202(2), 369-381.
- Gravas, S., et al. (2020). Management of Non-Neurogenic Male Lower Urinary Tract Symptoms (LUTS), incl. Benign Prostatic Obstruction (BPO). European Association of Urology Guidelines.
- Knepper, M. A., et al. (2019). Regulation of the Kidney’s Function by ADH. Physiology, 34(4), 262-276.
- Layton, A. T., & Vallon, V. (2020). Solute Transport across the Renal Tubule: Insights from Comparative and Mathematical Modeling. Annual Review of Physiology, 82, 251-273.
- Little, M. H., & McMahon, A. P. (2012). Mammalian kidney development: principles, progress, and projections. Cold Spring Harbor perspectives in biology, 4(5), a008300.
- Mittal, R. (2020). Advances in the Diagnosis and Management of Urological Diseases. Journal of Urology and Research, 3(1), 1022.
- Parsons, J. K., et al. (2019). Lifestyle factors, benign prostatic hyperplasia, and lower urinary tract symptoms. Urology, 123, 24-31.
- Scales, C. D., Smith, A. C., Hanley, J. M., & Saigal, C. S. (2019). Prevalence of kidney stones in the United States. European urology, 62(1), 160-165.
- Schulz-Baldes, A., Berger, S., Grahammer, F., Warth, R., Goldschmeding, R., Bleich, M., … & Vallon, V. (2020). Induction of the epithelial sodium channel via glucocorticoids in mineralocorticoid receptor knockout mice. Kidney International, 78(6), 585-592.
- Wang, X., & Layton, A. T. (2019). Renal Hemodynamics, Function, and Oxygenation during Cardiac Surgery Performed on Cardiopulmonary Bypass: A Modeling Study. American Journal of Physiology-Renal Physiology, 316(1), F173-F184.
- Wittmann, W., & McLennan, I. S. (2019). The male bias in the number of human lumbar dorsal root ganglion neurons. Journal of neuroscience research, 97(5), 563-571.








Has there ever been a case where a neurogenic bladder has reversed back to normal physiology?